Physical Address
8206 Louisiana Blvd NE, Suite A N03815
Albuquerque, NM 87113
United States
Physical Address
8206 Louisiana Blvd NE, Suite A N03815
Albuquerque, NM 87113
United States

Somewhere in your 50s or 60s, the narrative changes. Society starts lowering expectations for what your body should be capable of. But decline isn't inevitable—adaptation is. Active aging isn't about pretending you're 25. It's about understanding how your body changes and working with those changes intelligently. This complete guide covers everything you need to stay strong, mobile, and functional through your 50s, 60s, 70s, and beyond.
Somewhere in your 50s or 60s, the narrative changes. Doctors start talking about “age-appropriate” activities. Friends mention what they “can’t do anymore.” Society starts lowering expectations for what your body should be capable of.
Here’s what I’ve learned after watching countless people navigate aging—some successfully, others not: decline isn’t inevitable, but adaptation is necessary. The approach that worked in your 30s won’t work in your 60s. But that doesn’t mean settling for progressive limitation.
Active aging isn’t about pretending you’re 25. It’s about understanding how your body changes with age and working with those changes intelligently. It’s about maintaining strength, mobility, and function through your 50s, 60s, 70s, and beyond—not through heroic effort or denial, but through smart, sustainable practices.
I watched my uncle go from weekend tennis at 62 to barely walking at 68 because he stopped moving when his knee started hurting. ‘Protecting it,’ he said. Six years later, he needed a replacement that could’ve been delayed a decade with the right approach. That’s what this is about—not miraculous recovery, but intelligent adaptation that buys you years of function.

This guide covers everything I wish someone had told me and the people I care about before age-related joint problems became entrenched patterns. Not vague platitudes about “staying active,” but specific, actionable strategies backed by research and real-world results.
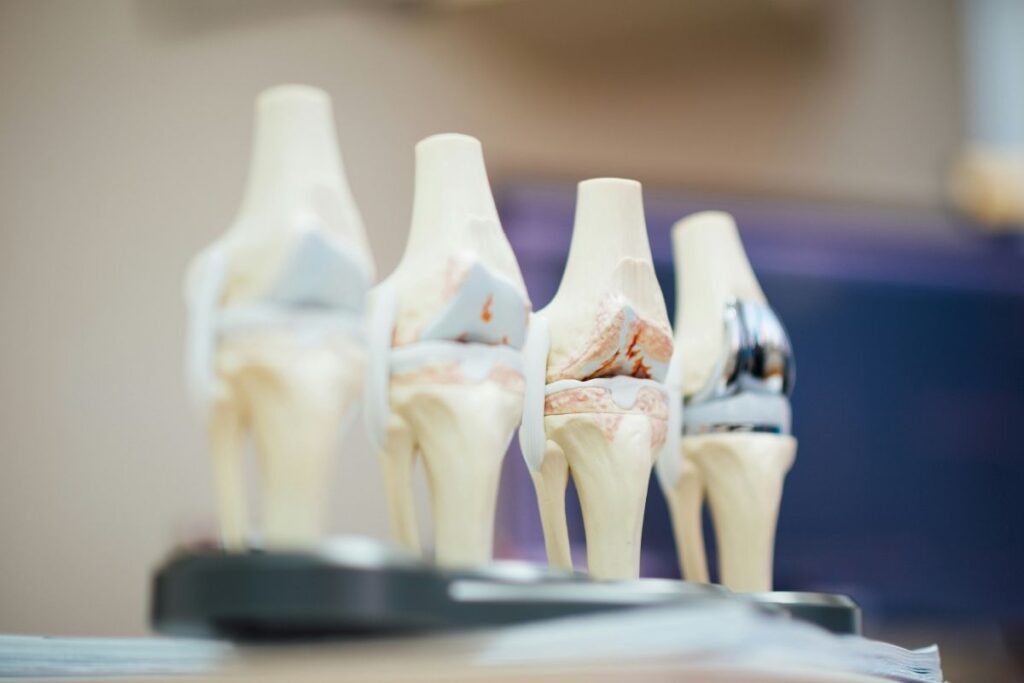
Understanding what’s normal versus what’s preventable changes how you approach aging.
Cartilage does thin with age. The smooth cushioning in your joints gradually loses thickness and resilience. This is normal, universal, and starts earlier than you think—by your 30s. But the rate varies enormously. Some 80-year-olds have minimal cartilage loss while some 50-year-olds have significant degeneration. The difference is usually decades of movement patterns, loading, and maintenance.
Muscle mass declines (sarcopenia) starting around age 30, accelerating after 50. Without intervention, you lose roughly 3-8% of muscle mass per decade after 30, more after 60. This matters because muscles stabilize joints, absorb force, and maintain movement quality. Weak muscles mean joints take more direct stress.
But here’s the critical point: this muscle loss is largely preventable and reversible with resistance training. You can build muscle at 70. It’s harder than at 30, requires more attention to recovery, but it absolutely works.
Bone density decreases, particularly after menopause in women. This increases fracture risk and can change how your skeleton handles load. Again, largely modifiable through weight-bearing activity and nutrition.
Connective tissue becomes less elastic. Tendons, ligaments, and fascia get stiffer and less pliable. Recovery from strains takes longer. Flexibility you used to have naturally now requires maintenance. This is real and needs adaptation—you can’t warm up the same way you did at 25.
Inflammation increases systemically (inflammaging). Background inflammation levels rise with age, contributing to joint pain, slower recovery, and various age-related diseases. This responds dramatically to lifestyle—diet, movement, sleep, stress management.
Proprioception declines. Your body’s awareness of where it is in space gets less precise. Balance suffers. Reaction time slows. This increases fall risk and joint injury susceptibility. Completely trainable through specific practices.
What doesn’t inevitably decline: your ability to be strong, mobile, functional, and active. These require more intentionality after 50 than before, but they’re absolutely maintainable with the right approach.
Most age-related joint problems are accelerated by predictable errors.
Becoming sedentary “to protect joints.” This is the most damaging mistake. People feel some joint pain, back off activity to avoid aggravation, and spiral into progressive weakness and stiffness. Joints need regular movement to stay healthy. Appropriate activity protects them; immobility accelerates decline.
I’ve watched this pattern countless times. Someone’s knee starts bothering them in their mid-50s. They stop walking as much, avoid stairs, quit activities they enjoyed. Within two years, they’ve lost significant leg strength, their knee is worse not better, and now their back hurts from compensation. The “protection” strategy backfired completely.
Continuing high-impact activities without adaptation. The opposite error—ignoring signals and pushing through like you’re still 30. Your 60-year-old joints can’t handle the same pounding as your 30-year-old joints. That doesn’t mean stop moving; it means adapt how you move.
Running five miles daily might have worked fine at 35. At 65, it might accelerate knee degeneration. Switching to three miles of walking plus strength training might preserve function far better.
Neglecting strength training. Cardio gets attention because it’s familiar and feels productive. But maintaining muscle mass and strength is far more critical for joint health and function after 50. Strong muscles are the difference between moving confidently and feeling fragile.
Ignoring mobility work. Flexibility and mobility naturally decline but are trainable. Most people do nothing about this until they can’t tie their shoes or reach overhead. Ten minutes of daily mobility work prevents years of progressive stiffness.
Eating like you’re 25. Metabolic rate slows, inflammation increases, and body composition shifts. The diet that maintained your weight at 30 causes weight gain at 60. Extra weight multiplies joint stress. Inflammatory foods that your younger body tolerated now drive pain and stiffness.
Accepting pain as inevitable. “It’s just aging” becomes an excuse to not address modifiable problems. Some age-related changes are real, but persistent pain usually indicates something addressable—movement pattern problems, strength imbalances, inflammatory diet, inadequate recovery.

Specific movement practices make the difference between healthy aging and progressive limitation.
Daily walking remains paramount. Not intense, not competitive—just consistent walking that loads joints appropriately, maintains cardiovascular health, and prevents the muscle atrophy that comes from sedentary life. Thirty to sixty minutes daily on varied terrain, paying attention to posture and gait.
As you age, surface matters more. Grass, dirt trails, and tracks are gentler than pavement. Hills build strength better than flat ground but downhill stresses knees more—choose routes thoughtfully.
I know people in their 70s who walk daily and move better than sedentary 50-year-olds. The walking itself is medicine, but only if done consistently.
Strength training becomes non-negotiable. This is the most important shift after 50. You need to actively build and maintain muscle or you’ll lose it progressively.
Strength training becomes even more important when joint discomfort shows up, especially in weight-bearing joints like the knees, where targeted knee exercises can significantly improve stability and reduce pain over time.
Focus on functional patterns—squats, hinges, pushes, pulls—not bodybuilder isolation work. You’re building strength to support real-life movement, not aesthetics. Moderate weights, controlled movement, two to three times weekly with adequate recovery.
The research is unequivocal: resistance training in older adults improves strength, bone density, balance, and functional capacity while reducing pain and injury risk. It’s not optional for healthy aging.
Mobility work fills gaps. Daily practice restoring and maintaining joint range of motion. This doesn’t mean aggressive stretching or forcing painful ranges. It means gentle, consistent work moving joints through their available range, gradually expanding it.
Morning mobility routines targeting hips, spine, shoulders, and ankles prevent the progressive stiffness that makes people move like they’re fragile. Ten to fifteen minutes daily is transformative over months.
Balance training prevents falls. Single-leg stands, tandem walking, stability exercises—these train the proprioceptive and vestibular systems that naturally decline. Falls are a leading cause of loss of independence in older adults. Balance training is insurance.
Low-impact alternatives replace high-impact activities. Swimming, cycling, elliptical, rowing—these maintain cardiovascular fitness without the joint stress of running. You can stay extremely fit without pounding your joints into early degeneration.
The specifics matter enormously for older adults.
Start with bodyweight or very light resistance. Even if you were strong when younger, your connective tissue needs time to adapt. Muscles respond relatively quickly to training; tendons and ligaments adapt slowly. Rushing this causes injuries that set you back months.
Begin with movements you can control perfectly—wall pushups, bodyweight squats to a chair, dead bugs, bird dogs, planks. Master control and stability before adding significant load.
Prioritize lower body. Leg strength determines mobility and independence. Your ability to stand from a chair, climb stairs, and prevent falls depends on leg strength. Squats, step-ups, lunges, deadlifts—these are foundational.
Upper body matters too, but if you have limited time, lower body takes priority.
Focus on eccentric control. The lowering phase of movements (eccentric) builds strength effectively and is particularly protective for older adults. Step-downs, slow lowering during squats, controlled descent on pushups—emphasize control during the lowering phase.
Recovery needs more attention. You can’t train hard multiple days in a row like you could at 30. Muscles need 48-72 hours between sessions targeting the same areas. Two to three full-body sessions weekly with rest days between works well.
Sleep, nutrition, and stress management become more critical for recovery as you age.
Form matters infinitely more than load. Perfect form with light weight builds strength safely. Heavy weight with poor form creates injuries. Nobody cares what you lift in your 60s. They care whether you can still move independently in your 80s.
Work with a knowledgeable trainer initially if possible. Learning proper movement patterns prevents years of doing things wrong that lead to pain and injury.
Progressive overload still applies. You need gradually increasing challenge to build strength. But progression is slower and more conservative. Add reps before weight. Add weight in smaller increments. Prioritize consistency over intensity.
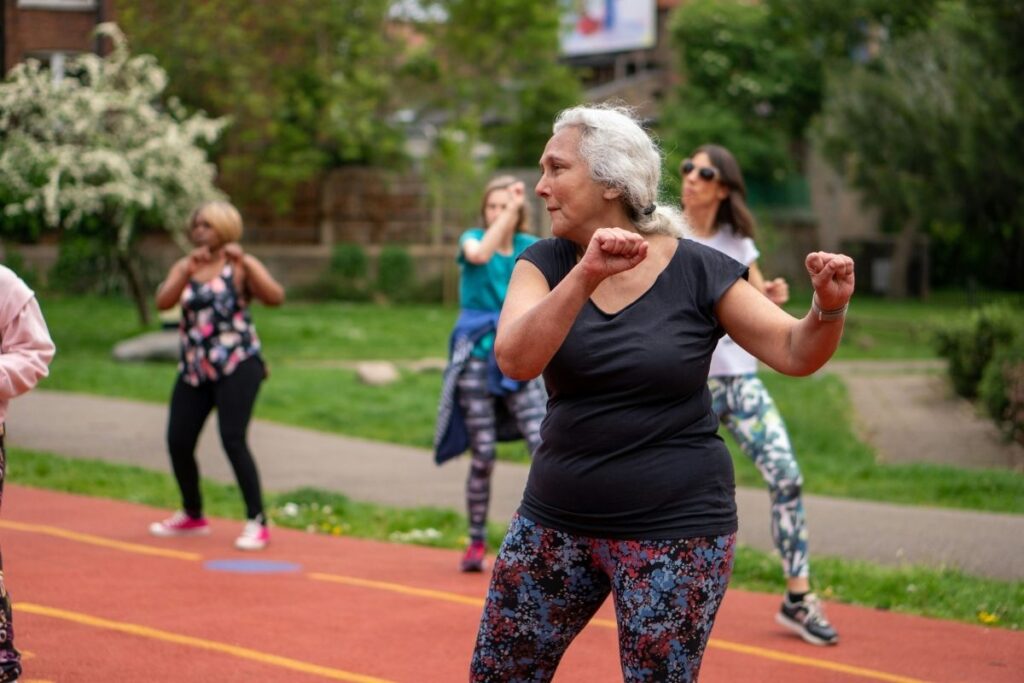
Mobility work prevents the progressive stiffness that defines aging for many people.
Morning routines set the tone. Your joints are stiff after hours of immobility during sleep. Five to ten minutes of gentle movement before launching into your day prevents that stiff, achy feeling from persisting.
Neck rolls, shoulder circles, spinal rotations, hip circles, ankle mobility—simple movements through available range, done smoothly without force. This gets synovial fluid moving, warms tissues, and signals your nervous system that movement is safe.
Hip mobility is critical. Tight hips change how you walk, stress your knees and back, and limit functional movement. Daily hip mobility work—figure-four stretches, hip circles, 90-90 position work—maintains the hip range needed for comfortable movement.
I’ve seen tight hips contribute to more knee and back problems than almost anything else in older adults. Fifteen minutes of daily hip work prevents years of compensation patterns.
Spinal mobility prevents back pain. Your spine naturally loses range with age, particularly rotation. Cat-cow movements, gentle spinal twists, thoracic extension over a foam roller—these maintain the spinal mobility that allows comfortable, pain-free movement.
Ankle mobility affects everything above. Stiff ankles change how your foot strikes during walking, alter knee tracking, and limit squat depth. Simple ankle circles and calf stretches maintain the range needed for normal gait.
Shoulder mobility preserves function. Reaching overhead, behind your back, across your body—these ranges decline without maintenance. Daily shoulder circles, wall slides, and doorway stretches keep shoulders functional for dressing, reaching, and lifting.
The pattern: daily, gentle, consistent mobility work prevents progressive stiffness. It’s not dramatic, doesn’t produce immediate results, but accumulates into maintained function over years.

What you eat matters more as you age, not less.
Protein needs increase. Older adults need more protein to maintain muscle mass—roughly 1.2-1.6 grams per kilogram body weight versus the 0.8 g/kg often recommended. Spread protein across meals; your body can only use so much at once.
Without adequate protein, strength training can’t build muscle effectively. You’re giving your body a stimulus without the building materials to respond.
Anti-inflammatory eating reduces joint pain. The Mediterranean diet pattern—high in fish, vegetables, olive oil, nuts, moderate wine—consistently shows reduced inflammation and slower arthritis progression in research.
Reducing processed foods, excess sugar, and omega-6 vegetable oils while increasing omega-3s, colorful vegetables, and polyphenols measurably affects inflammatory markers and joint symptoms.
Maintain healthy weight. Every pound of excess weight multiplies force on knees and hips. Losing modest weight—even 10-15 pounds—significantly reduces joint pain and slows cartilage loss in research studies.
Weight management gets harder with age due to metabolic slowdown. You can’t eat the same amount you did at 30 and maintain weight at 60. Adaptation is necessary.
Stay hydrated. Dehydration affects joint lubrication and recovery. Older adults often have decreased thirst signals but still need adequate water. Half your body weight in ounces daily is a reasonable target.
Key micronutrients matter. Vitamin D (most older adults are deficient), calcium (for bone health), omega-3s (anti-inflammatory), and magnesium (muscle and nervous system function) deserve attention through diet or supplementation if needed.
Collagen and bone broth provide building blocks. While evidence is mixed, many people report improved joint comfort with daily collagen supplementation. It’s low-risk and potentially beneficial.
Alongside movement and strength work, addressing inflammation through nutrition and evidence-based supplements like curcumin from turmeric can support joint comfort as we age.
Pain management without over-reliance on medications requires a comprehensive approach.
Movement, not rest, is usually the answer. When joints hurt, the instinct is rest. Short-term rest for acute pain is fine. But extended rest weakens muscles and stiffens joints, making pain worse.
Gentle movement—walking, swimming, tai chi—often reduces pain better than inactivity by maintaining circulation, clearing inflammatory mediators, and preventing stiffness.
Heat before activity, ice after inflammation. Heat before movement warms tissues and reduces stiffness. Ice after activity that causes swelling helps control inflammation. This simple pattern manages symptoms without medication for many people.
Targeted supplements help. Omega-3s, curcumin, glucosamine (for some people), and possibly collagen all have evidence supporting pain reduction and inflammation control. They’re not miracle cures but legitimate tools in a comprehensive approach.
Sleep quality directly affects pain. Poor sleep increases inflammatory markers and lowers pain tolerance. Prioritizing sleep—dark room, consistent schedule, limited screens before bed—measurably improves pain levels.
Stress management matters. Chronic stress elevates cortisol and inflammatory cytokines, worsening pain. Whatever stress reduction works for you—meditation, time in nature, therapy, social connection—is worth prioritizing.
NSAIDs strategically, not habitually. Occasional use for acute pain is fine. Daily long-term use carries real risks—stomach problems, kidney issues, cardiovascular concerns. Save them for when you genuinely need them rather than using them preventively.

Falls are the leading cause of injury-related deaths in adults over 65. Prevention is critical.
Single-leg balance training works. Stand on one leg while brushing teeth, washing dishes, or waiting for coffee. Work up to 30-60 seconds per leg without wobbling. This trains the stabilizing muscles and proprioceptive systems that prevent falls.
Tandem walking improves stability. Walk heel-to-toe in a straight line. Harder than it sounds, and directly trains balance needed for uneven terrain and unexpected perturbations.
Tai chi reduces fall risk. Research consistently shows that tai chi practice improves balance, reduces fall rates, and increases confidence in older adults. The slow, controlled movements train stability in multiple directions.
Strength training improves balance. Strong legs and core provide the foundation for stability. Single-leg exercises, step-ups, and controlled movements train both strength and balance simultaneously.
Vision and foot health matter. Get vision checked regularly—poor vision increases fall risk. Maintain foot strength and flexibility. Wear appropriate shoes with good ground feel rather than thick-soled shoes that reduce sensory feedback.
Home safety reduces risk. Remove tripping hazards, improve lighting, add grab bars where needed. The environment contributes significantly to fall risk.
You don’t have to give up activities as you age, but adaptation might be necessary.
Running to walking. Many lifelong runners eventually need to transition. This doesn’t mean fitness loss—walking maintains cardiovascular health and reduces joint stress. Some mix running shorter distances with longer walks.
Heavy lifting to moderate resistance. You can stay strong without maxing out barbells. Moderate weights with perfect form build and maintain strength safely.
High-impact sports to modified versions. Tennis becomes pickleball or doubles tennis. Basketball becomes shooting around. Soccer becomes walking soccer. You stay active and social without the injury risk.
Longer warm-ups and recovery. Activities that required five minutes of warm-up at 30 might need fifteen minutes at 60. Recovery between sessions extends. Adaptation isn’t failure; it’s intelligence.
Focus shifts from performance to participation. Competitive goals give way to sustainability goals. Instead of running your fastest 5K, you run consistently without pain. Instead of lifting your heaviest weights, you train in ways you can maintain for decades.
This isn’t resignation. It’s choosing long-term participation over short-term performance—a trade that pays dividends.
Physical practices matter, but so does mindset and community.
Stay socially active. Isolation increases mortality risk as much as smoking. Group exercise classes, walking groups, sport leagues—the social connection matters as much as the physical activity.
Maintain purpose and challenge. People who stop challenging themselves mentally and physically decline faster. Set goals—complete a hike, learn a new activity, achieve a strength milestone. Purpose drives action.
Reframe limitations as adaptations. Needing to modify activities isn’t failure. It’s intelligent response to changing capabilities. People who adapt successfully maintain quality of life far longer than those who rigidly cling to past approaches.
Build confidence through small wins. Progressive improvement—even modest—builds the confidence that prevents the fragility mindset. Track strength gains, mobility improvements, pain reductions. Evidence of capability combats narratives of inevitable decline.
Everyone’s starting point and goals differ. Here’s a framework to build your approach:
Assess current state honestly:
Set specific, achievable goals:
Build your weekly structure:
Start conservatively and progress gradually: Week 1-4: Establish consistency at easy level Week 5-8: Gradually increase challenge Month 3+: Continue progressive overload while maintaining consistency
Track what matters:
Adjust based on feedback:

Active aging is a decades-long commitment, not a 12-week program.
The practices that keep you mobile and functional at 60 need to continue at 70, 80, and beyond. They’ll evolve—lighter weights, gentler approaches, more recovery—but the fundamentals remain: move regularly, maintain strength, preserve mobility, manage inflammation, stay socially engaged.
I’ve seen people in their 70s who move better than sedentary 50-year-olds because they’ve maintained these practices consistently. I’ve also seen 60-year-olds who’ve let decline become their story, accepting limitation as inevitable when it was largely preventable.
The trajectory isn’t fixed. Where you are now doesn’t determine where you’ll be in 10 years. Consistent, intelligent practices change outcomes profoundly.
Your joints have carried you this far. With proper care, attention, and adaptation, they can continue carrying you well for decades more. Not without any changes—adaptation is necessary—but without the dramatic decline many accept as normal.
Active aging isn’t about denying reality. It’s about refusing to accept unnecessary limitation. It’s about maintaining the strength, mobility, and function that let you keep doing what matters to you.
That’s worth the daily commitment.
Note: This is comprehensive educational information, not medical advice. Work with healthcare providers and qualified trainers to develop a personalized plan appropriate for your specific situation, health conditions, and capabilities.