Physical Address
8206 Louisiana Blvd NE, Suite A N03815
Albuquerque, NM 87113
United States
Physical Address
8206 Louisiana Blvd NE, Suite A N03815
Albuquerque, NM 87113
United States
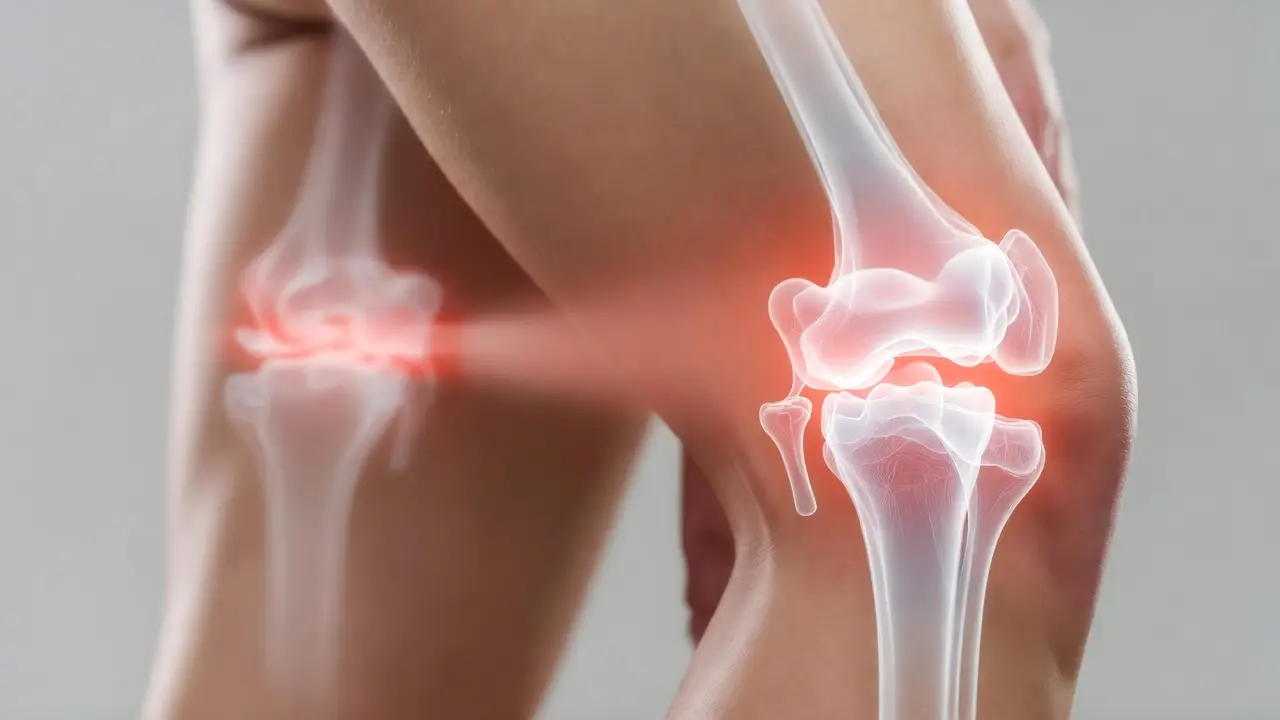
Your joints are the unsung heroes of daily life until they start complaining. Most people only care about joint health after damage is done. That's backwards. Understanding how joints work and what keeps them healthy prevents years of pain. I've spent thousands of hours researching what separates people who maintain function into their 80s from those who decline. The patterns are clear. This guide reveals the seven essential principles that determine joint health outcomes.
Your joints are the unsung heroes of daily life. You don’t think about them until they start complaining—a knee that clicks going down stairs, hands that feel stiff in the morning, a hip that aches after sitting too long.
Most people only start caring about joint health after damage is done. That’s backwards. Understanding how joints actually work and what keeps them healthy prevents years of unnecessary pain and limitation.
This reactive mindset is one of the biggest reasons people struggle later in life, which is why understanding the principles of active aging after 50 is so critical for preserving long-term joint function.
I’ve spent thousands of hours researching joint health, testing approaches on myself, and watching what separates people who maintain function into their 70s and 80s from those who progressively decline. The patterns are clear. Joint health isn’t mysterious or complicated, but it does require understanding a few fundamental principles that most people never learn.
This guide breaks down the seven essential principles that determine whether your joints stay healthy or deteriorate. Not vague advice about “staying active.” Specific, actionable strategies backed by research and proven through real-world results.
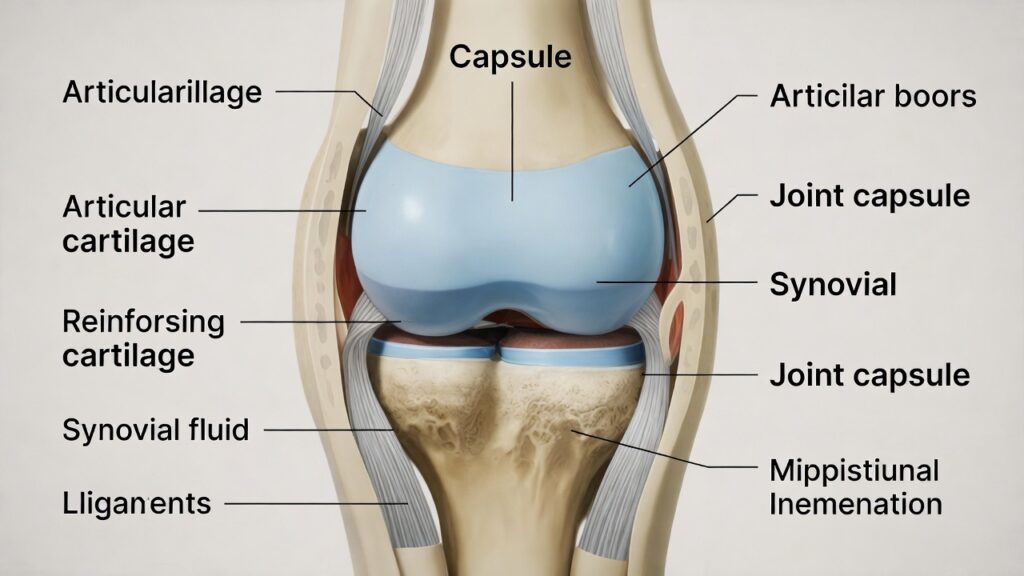
Before we dive into specific principles, let’s establish what joint health actually means.
Healthy joints move smoothly through their full range without pain or restriction, supported by cartilage, synovial fluid, and surrounding structures—factors consistently highlighted by the Arthritis Foundation as essential to long-term joint health.
The cartilage cushioning bone ends stays thick and resilient. Synovial fluid lubricates surfaces effectively. Supporting muscles provide stability. Ligaments maintain proper alignment. Inflammation stays minimal.
When any of these elements break down, joint health deteriorates. Cartilage thins. Fluid quality decreases. Muscles weaken. Inflammation increases. Movement becomes painful and restricted.
The good news? Most joint health factors are within your control. Genetics matter, but lifestyle choices matter more. The trajectory isn’t fixed—what you do daily determines outcomes more than age or family history.

This is the foundation everything else builds on. Your joints need regular movement to stay healthy.
Cartilage has no blood supply. It gets nutrients through compression and release as you move—like squeezing a sponge. When you walk, climb stairs, or exercise, you’re literally feeding your cartilage. Immobility starves it.
Synovial fluid also needs movement. Static positions allow it to thicken and settle. Movement keeps it flowing and distributing properly throughout the joint.
But movement quality matters as much as quantity. Poor movement patterns—limping, compensating, using joints in ways they’re not designed for—creates abnormal stress that accelerates wear. Good movement patterns distribute forces evenly and maintain joint health.
What this looks like practically:
Walking daily remains the gold standard for joint health. Thirty to sixty minutes of walking provides appropriate loading, maintains cardiovascular health, and prevents the muscle atrophy that compromises joint stability. Not intense, not competitive—just consistent walking with good posture and natural gait.
Strength training becomes increasingly important after age 40. Strong muscles stabilize joints and reduce load on cartilage. Two to three sessions weekly focusing on functional movements—squats, hinges, pushes, pulls—builds the strength that protects joints.
For joints like the knees, targeted strengthening work matters even more, which is why specific knee exercises play a major role in protecting joint health and preventing long-term deterioration.
Mobility work prevents the progressive stiffness many accept as normal aging. Ten to fifteen minutes daily of gentle stretching and range of motion exercises maintains flexibility and prevents compensatory movement patterns.
The pattern: regular, varied movement done with good mechanics. Not occasional intense sessions, not complete rest, but consistent moderate activity that keeps joints functioning optimally.
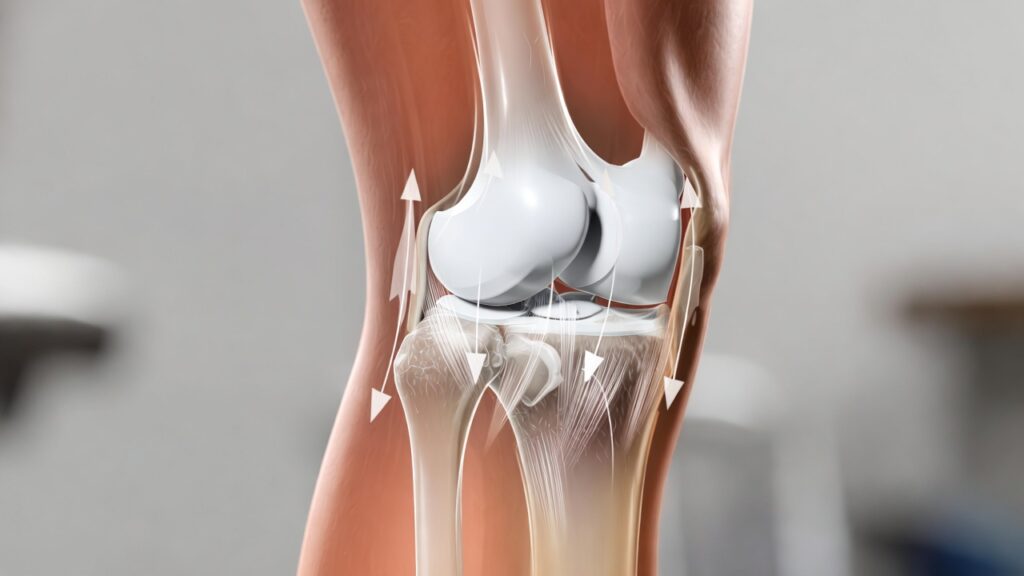
Every pound of body weight multiplies force on your joints with each step. The exact multiplication factor varies by joint and activity, but for knees during walking, each pound creates roughly four pounds of force.
This means losing ten pounds effectively removes forty pounds of force from your knees with every step. Over thousands of steps daily, this accumulation becomes enormous.
The research is unambiguous: excess weight accelerates cartilage breakdown in weight-bearing joints, with findings supported by studies published through the National Institutes of Health — knees, hips, ankles, spine. It also increases systemic inflammation, which affects all joints including hands and shoulders.
Weight loss, even modest amounts, measurably reduces pain and slows joint health deterioration. Studies consistently show that losing 10-15 pounds produces significant improvements in knee osteoarthritis symptoms and function.
Beyond just mechanics:
Fat tissue isn’t inert. It produces inflammatory compounds called adipokines that circulate throughout your body, contributing to joint inflammation and cartilage breakdown. This is why weight affects hand joints despite them not bearing body weight directly.
Metabolic health ties into joint health through multiple pathways. Insulin resistance, diabetes, and metabolic syndrome all increase joint problems independent of mechanical loading. Managing these conditions protects joints beyond just weight reduction.
The practical approach:
You don’t need dramatic weight loss to see joint health benefits. Even five to ten percent of body weight makes measurable differences. A 200-pound person losing 10-20 pounds will likely notice significant improvement in knee and hip comfort.
Focus on sustainable changes rather than aggressive diets. Gradual weight loss maintained long-term beats rapid loss that rebounds. The goal is permanent habit change, not temporary restriction.

What you eat directly influences inflammation levels throughout your body, including your joints.
Chronic low-grade inflammation contributes to cartilage breakdown, pain, and progressive joint deterioration. Certain dietary patterns consistently reduce inflammatory markers while others reliably increase them.
Alongside dietary patterns, certain compounds—such as curcumin from turmeric — have been shown to support inflammation management and may complement a joint-friendly lifestyle.
The Mediterranean eating pattern has the strongest evidence for reducing inflammation and supporting joint health, with research summarized by Harvard Health showing consistent reductions in inflammatory markers.
This isn’t just correlation—mechanistic studies show how specific foods influence inflammatory pathways. Omega-3 fatty acids from fish compete with omega-6 fatty acids in inflammatory processes, shifting the balance toward less inflammation. Polyphenols from colorful vegetables and fruits have direct anti-inflammatory and antioxidant effects.
Specific foods that matter for joint health:
Fatty fish (salmon, mackerel, sardines) provide EPA and DHA omega-3s that measurably reduce joint inflammation. Two to three servings weekly make a difference.
Extra virgin olive oil contains oleocanthal, which works similarly to ibuprofen by inhibiting inflammatory enzymes. Using it liberally as your primary fat supports joint health.
Colorful vegetables and berries provide polyphenols with anti-inflammatory effects. Variety matters—different colors provide different beneficial compounds.
What to minimize:
Processed foods high in refined carbohydrates and added sugars spike blood sugar and insulin, triggering inflammatory responses.
Excessive omega-6 vegetable oils (soybean, corn, safflower) shift inflammatory balance in the wrong direction. They're not evil, but modern diets are heavily skewed toward omega-6.
Trans fats and highly processed seed oils contribute to inflammation. Minimize these where possible.
The pattern: whole foods rich in omega-3s, polyphenols, and fiber. Minimal processed foods, excess sugar, and inflammatory fats. This eating approach supports joint health while benefiting overall health simultaneously.

Weak muscles mean joints absorb more direct stress. Strong muscles act as shock absorbers and stabilizers, distributing forces more evenly and reducing load on cartilage.
This relationship is particularly clear in knees. Quadriceps strength directly correlates with knee joint health. People with stronger quads have less pain, better function, and slower cartilage loss than those with weak quads, even when starting with the same degree of arthritis.
Hip and gluteal strength matters enormously for both hip and knee joint health. Weak glutes cause knee valgus (inward collapse) during movement, creating abnormal stress patterns that accelerate wear. Strong glutes keep knees tracking properly and reduce hip joint stress.
Core strength protects the spine. Weak core muscles force spinal joints to work harder to maintain stability, accelerating disc degeneration and facet joint problems.
The implications:
Strength training isn’t optional for long-term joint health. It’s foundational. You can eat perfectly, maintain ideal weight, and take every supplement—if your muscles are weak, your joints will deteriorate faster.
The good news: you don't need to be a powerlifter. Moderate strength maintained consistently protects joints. Two to three sessions weekly of functional strength training—focusing on movements, not muscles—builds sufficient strength.
Bodyweight exercises work initially. Squats, lunges, pushups, planks, step-ups. As you adapt, add moderate resistance through bands, dumbbells, or machines. The goal is progressive overload over months and years, not maximal lifts.
Form matters infinitely more than load. Perfect control with light weight beats heavy weight with poor mechanics. You’re building joint-protective strength, not competing in powerlifting.
Joints require a balance between stability (strength and control) and mobility (range of motion and flexibility).
Too much mobility without stability creates hypermobility and joint instability. The joint moves through large ranges but lacks control, leading to injuries and accelerated wear.
Too much stability without mobility creates stiffness and restricted movement. You’re strong but can’t move through necessary ranges, forcing compensatory patterns that stress other joints.
Healthy joint health maintains both. Sufficient strength and neuromuscular control to stabilize joints during movement, combined with adequate flexibility and range to move through functional patterns.
Different joints need different balances:
Some joints are built primarily for stability—your spine, for example. These need strength and control more than extreme flexibility.
Others are built for mobility—shoulders and hips. These need both strength throughout large ranges and maintained flexibility.
Knees and elbows are hinge joints—they need stability in most planes but good flexion-extension range.
Understanding what your specific joints need prevents both overtraining flexibility where stability matters and neglecting mobility where range is crucial.
Practically implementing this:
Daily mobility work maintains range in joints that naturally stiffen—hips, thoracic spine, shoulders, ankles. Ten to fifteen minutes of gentle stretching and movement through available ranges.
Strength training that moves through full ranges builds both stability and mobility simultaneously. Deep squats, overhead presses, rows through full range—these develop functional strength while maintaining mobility.
Balance and proprioception training improves joint stability. Single-leg exercises, balance challenges, unstable surface work—these train the neuromuscular control that keeps joints stable.

Recovery is when adaptation happens. You don’t get stronger or healthier during exercise—you get stronger during recovery from exercise.
Sleep particularly matters for joint health through several mechanisms:
Growth hormone release during deep sleep supports tissue repair, including cartilage. Poor sleep disrupts this process.
Inflammatory regulation depends heavily on sleep. Sleep deprivation increases inflammatory markers throughout your body, worsening joint inflammation and pain.
Pain perception changes with sleep quality. Poor sleep lowers pain tolerance, making joint discomfort feel worse even if actual tissue damage hasn’t changed.
The research consistently shows that people with poor sleep have worse joint pain, higher inflammatory markers, and faster progression of arthritis compared to those sleeping adequately.
Beyond sleep:
General recovery practices matter. Overtraining without adequate recovery breaks down joints faster than building them up. Rest days between training sessions allow adaptation.
Stress management influences joint health through cortisol and inflammatory pathways. Chronic stress elevates inflammation and worsens pain independent of physical factors.
Hydration affects joint lubrication. Synovial fluid quality depends on adequate hydration. Dehydration makes joints feel stiffer and less comfortable.
Making this practical:
Prioritize seven to nine hours of sleep nightly. Not aspirational—actual sleep. Dark room, cool temperature, consistent schedule, limited screens before bed.
Build rest days into your training schedule. Hard training days should alternate with lighter activity or complete rest. More isn’t always better.
Find stress management that actually works for you—meditation, nature time, therapy, whatever reduces your stress load. This isn’t optional wellness fluff; it’s joint health medicine.
Small problems become big problems when ignored. Early-stage joint issues respond well to conservative interventions. Advanced problems often require aggressive treatment.
The window for preventing progression is real and limited. Early osteoarthritis responds to exercise, weight loss, and lifestyle modification. Advanced osteoarthritis with severe cartilage loss may require surgery.
Early tendonitis resolves with rest and modified activity. Chronic tendinopathy with structural degeneration takes months of rehabilitation.
Recognizing early warning signs and responding appropriately prevents years of progressive decline:
Warning signs to address promptly:
Morning stiffness lasting more than a few minutes suggests inflammatory processes starting. This is the time to address diet, sleep, and activity patterns—not years later when damage is extensive.
Pain with specific activities indicates mechanical stress exceeding tissue tolerance. Modify the activity, address biomechanical issues, build supporting strength before damage accumulates.
Reduced range of motion develops gradually but indicates joint changes. Daily mobility work prevents progressive stiffness from becoming permanent restriction.
Persistent swelling suggests ongoing inflammation. This needs investigation and management, not just pain medication to mask symptoms.
The intervention hierarchy:
First line: lifestyle modification. Movement patterns, weight management, anti-inflammatory eating, sleep optimization. These address root causes.
Second line: conservative treatments. Physical therapy, targeted exercises, quality supplements, appropriate use of anti-inflammatories.
Third line: medical interventions. Injections, procedures, medications when conservative approaches prove insufficient.
Fourth line: surgery when joint damage is severe enough that quality of life is significantly impaired despite maximal conservative treatment.
Most people skip straight to medications or eventually surgery without exhausting conservative options. This is backwards. The earlier you intervene with lifestyle approaches, the better your long-term outcomes.
These seven principles work synergistically. Focusing on one while ignoring others produces suboptimal results.
Movement without weight management means excessive load on joints despite good activity. Weight loss without strength training leaves joints unsupported and vulnerable. Strong muscles with poor mobility create compensatory patterns and stiffness.
The most effective approach addresses all principles simultaneously:
Daily practices:
Weekly practices:
Ongoing priorities:
Quarterly reviews:
This isn’t complicated but it does require consistency. Joint health is built through daily choices compounded over months and years, not through occasional heroic efforts.
Understanding these principles empowers you to maintain joint health independently. But certain situations warrant professional evaluation:
Persistent pain despite appropriate lifestyle modification suggests something needing assessment. Don’t suffer unnecessarily when treatable issues exist.
Sudden onset of severe pain, swelling, or inability to move a joint requires prompt medical evaluation to rule out serious problems.
Progressive worsening despite your best efforts means something isn’t being addressed adequately. Professional guidance helps identify what’s being missed.
Wanting optimal individualized programming benefits from working with qualified physical therapists or trainers who can assess your specific movement patterns, strength imbalances, and joint mechanics.
Professional help complements self-management, not replaces it. The most successful outcomes combine professional guidance with personal commitment to implementing these foundational principles.
Joint health is a marathon, not a sprint. What you do today might not produce immediate results, but it determines outcomes years from now.
People who consistently apply these principles—appropriate movement, healthy weight, anti-inflammatory eating, adequate strength, good sleep—maintain remarkable joint function into their 70s and 80s.
People who ignore these principles progressively decline regardless of genetics or luck. Poor habits compound into poor outcomes just as surely as good habits compound into sustained function.
The trajectory isn’t fixed. Where you are now doesn’t determine where you’ll be in ten years. Consistent application of these seven principles changes outcomes profoundly.
Your joints have carried you this far. With proper care and attention built on these fundamental principles, they can continue carrying you well for decades more. Not without any changes—adaptation is necessary—but without the dramatic decline many accept as inevitable.
That’s the promise of understanding and implementing genuine joint health principles. Not miracle cures or quick fixes, but sustainable practices that maintain function for life.
Note: This is educational information about joint health fundamentals, not medical advice. Work with qualified healthcare providers for diagnosis and treatment of specific joint conditions or concerns.