Physical Address
8206 Louisiana Blvd NE, Suite A N03815
Albuquerque, NM 87113
United States
Physical Address
8206 Louisiana Blvd NE, Suite A N03815
Albuquerque, NM 87113
United States

The natural remedies market for joint pain drowns in noise—exotic herbs, magnetic bracelets, crystal healing. Most are wishful thinking. But buried in that noise are natural remedies that genuinely work, backed by research. I've spent years separating legitimate options from marketing hype. This guide focuses exclusively on natural remedies for joint pain with solid evidence. Not miracle cures, but interventions that provide genuine relief as part of comprehensive approaches.
The natural remedies market for joint pain is drowning in noise. Search online and you’ll find hundreds of products promising relief—essential oils, magnetic bracelets, exotic herbs, alkaline water, crystal healing, and supplements with ingredients you can’t pronounce.
Most are somewhere between wishful thinking and outright fraud. But buried in that noise are natural remedies for joint pain that genuinely work, backed by actual research and real-world results.
I’ve spent years separating legitimate options from marketing hype. Testing approaches on myself, reading through hundreds of studies, tracking outcomes with people using these remedies. The distinction matters enormously—wasting time and money on ineffective treatments delays real relief and allows problems to worsen.
This guide focuses exclusively on natural remedies for joint pain with solid evidence supporting their use. Not anecdotes or ancient wisdom, but interventions with mechanisms we understand and research demonstrating effectiveness. Some work through reducing inflammation, others through pain modulation, still others through supporting tissue repair.
None are miracle cures. Natural remedies work best as part of comprehensive approaches including appropriate movement, weight management, and addressing root causes. But within that context, these fifteen options provide genuine relief for many people without the side effects and risks of long-term pharmaceutical use.
Before diving into specific remedies, let’s establish realistic expectations and understand how to evaluate natural approaches.
"Natural" doesn't automatically mean safe or effective. Arsenic is natural. So is poison ivy. The question isn't whether something is natural—it's whether it works and whether benefits outweigh risks.
The natural remedies included here meet several criteria: mechanisms that make biological sense, research demonstrating effects beyond placebo, safety profiles allowing use without significant risk, and practical implementation that people can sustain.
Natural remedies work best as part of a broader strategy that includes appropriate movement, mobility training, and joint-supporting exercises designed to maintain long-term function.
Many work through reducing inflammation—the common pathway underlying most joint pain. Others provide building blocks for tissue repair or affect pain perception through nervous system modulation.
Individual responses vary. What works remarkably for one person might be minimally effective for another. This necessitates some experimentation guided by evidence about what’s most likely to help.
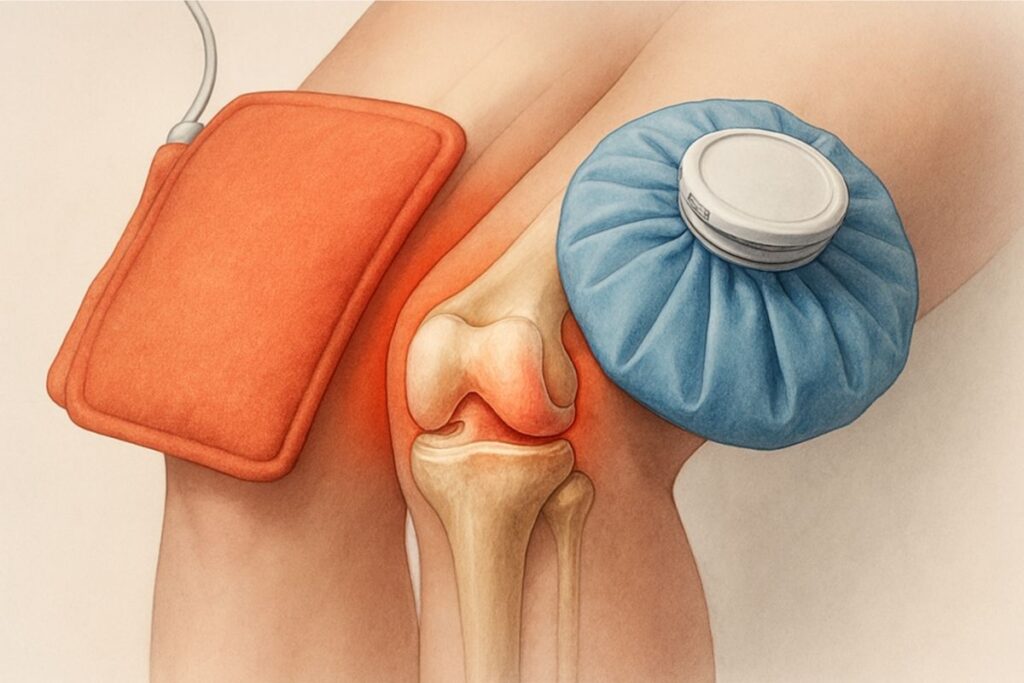
Heat is probably the most accessible natural remedy for joint pain, and it genuinely works through well-understood mechanisms.
How heat helps joint pain:
Heat increases blood flow to treated areas, delivering oxygen and nutrients while removing metabolic waste products. This supports healing and reduces the aching associated with poor circulation.
Warmth relaxes muscles surrounding joints. Muscle tension often accompanies and exacerbates joint pain—relaxing this tension reduces overall discomfort.
Heat improves tissue extensibility, making joints and surrounding structures feel less stiff. This is why hot showers in the morning reduce that “creaky” feeling many experience upon waking.
Heat also has direct effects on pain perception, activating thermal receptors that can temporarily override pain signals through gate control mechanisms.
Practical application:
Heating pads applied for 15-20 minutes before activity prepare stiff joints for movement. This is particularly effective for morning stiffness or before exercise.
Hot baths or showers provide whole-body heat exposure that’s especially beneficial for multiple affected joints. Adding Epsom salts may provide additional magnesium absorption, though evidence for this is limited.
Moist heat (hot towels, warm baths) penetrates deeper than dry heat (heating pads) for some people, though both are effective.
When to use heat:
Before activities requiring joint movement—exercise, extended walking, household tasks. Heat prepares joints and reduces discomfort during activity.
For chronic stiffness and aching without acute inflammation. Heat works well for osteoarthritis pain and general joint stiffness.
When to avoid heat:
Don’t use heat on acutely inflamed joints—hot, red, swollen joints with active inflammation. Heat increases inflammation in these cases. Use ice instead.
Don’t apply heat immediately before athletic activity requiring maximal performance—it can temporarily reduce muscle force production.
Ice and cold work through different mechanisms than heat, making them appropriate for different situations.
How cold helps joint pain:
Cold constricts blood vessels, reducing blood flow to treated areas. This limits the inflammatory response after injury or aggravation.
Numbing effects from cold temporarily reduce pain perception. The cold sensation overwhelms pain signals through neural mechanisms.
Cold reduces metabolic activity in tissues, decreasing the secondary damage that can occur after initial injury.
Swelling decreases with cold application, reducing pressure on surrounding tissues and pain receptors.
Practical application:
Ice packs wrapped in towels (never directly on skin) applied for 15-20 minutes after activities that cause joint swelling. This controls the inflammatory response.
Ice massage—rubbing an ice cube in circles over a painful joint—provides both cold therapy and mechanical stimulation. Seven to ten minutes per area.
Cold gel packs stored in freezers provide convenient, reusable cold therapy. Mold to joint contours better than ice packs.
Alternating cold and heat (contrast therapy) works for some people, though evidence is mixed. Try three minutes cold, three minutes heat, repeated three to four times.
When to use cold:
After activities that cause joint swelling—long walks, sports, extended standing. Cold controls inflammatory response.
For acutely painful, hot, swollen joints with active inflammation. Cold reduces inflammation better than heat in these situations.
When to avoid cold:
Before activity requiring joint movement—cold temporarily reduces joint proprioception and range of motion, potentially increasing injury risk.
If you have circulatory problems or cold sensitivity conditions like Raynaud’s disease. Check with doctors in these cases.

Capsaicin—the compound making chili peppers hot—provides legitimate pain relief when applied topically, though it works differently than you might expect.
How capsaicin works:
Capsaicin depletes substance P, a neuropeptide that transmits pain signals from nerves to your brain. With repeated application, nerve endings have less substance P available to signal pain.
This process takes time—several days to weeks of consistent application before maximal effects develop. Initial applications often increase burning sensations before improvement occurs.
Research supporting capsaicin:
Multiple studies show that topical capsaicin creams reduce osteoarthritis pain, particularly in hands and knees. One meta-analysis found significant pain reduction compared to placebo, with effects comparable to topical NSAIDs for some people.
The effectiveness relates to concentration—higher concentration products (0.075-0.1%) work better than lower concentrations, though they also cause more initial burning.
Practical use:
Apply capsaicin cream to affected joints 3-4 times daily. Consistency matters—sporadic use produces minimal benefit.
Wash hands thoroughly after application. Capsaicin burns sensitive tissues—eyes, nose, mouth, genitals. Avoid touching these areas after applying.
Initial burning sensation is normal and usually decreases after several days of regular use. If it’s intolerable, start with lower concentration products.
Cover applied areas with loose clothing to prevent accidentally touching and transferring to sensitive areas.
Who benefits most:
People with hand or knee osteoarthritis often see good results. The research for these specific joints is strongest.
Those seeking alternatives to oral pain medications without systemic side effects.
Important considerations:
Don’t apply to broken skin or open wounds. Don’t use heating pads on areas treated with capsaicin—this can intensify burning significantly.
Effects are temporary—capsaicin works as long as you continue using it. Stopping application means substance P levels recover and pain returns.
Arnica is an herb with genuine anti-inflammatory and analgesic properties when applied topically. The evidence is stronger for acute injuries than chronic pain.
Research on arnica:
Studies show topical arnica reduces pain and inflammation after acute injuries, sprains, and surgeries. A systematic review found it comparable to topical NSAIDs for some applications.
The mechanism involves sesquiterpene lactones in arnica that have anti-inflammatory effects and may reduce bruising by affecting blood vessel permeability.
Practical application:
Arnica gels or creams applied to affected areas 2-3 times daily. Start as soon as possible after injury for best results.
Arnica is most effective for acute injuries—sprains, bruises, post-surgical swelling—rather than chronic joint pain. Use it in the first days to weeks after injury.
Homeopathic arnica preparations are different from herbal arnica. The evidence is for herbal concentrations, not homeopathic dilutions. Check what you’re buying.
Who benefits:
People with acute joint injuries or flares. Athletes dealing with bruising and soft tissue injuries. Those recovering from joint procedures or surgeries.
Safety notes:
Don’t apply to broken skin. Some people develop allergic reactions—test on a small area first.
Don’t take arnica internally unless specifically formulated for that use—the herb can be toxic when ingested in significant amounts.
Willow bark is essentially natural aspirin—it contains salicin, which your body converts to salicylic acid, the active compound in aspirin.
How willow bark works:
Salicin inhibits COX enzymes that produce inflammatory prostaglandins, similar to how aspirin and other NSAIDs work. This reduces both inflammation and pain.
The effects are milder than pharmaceutical NSAIDs but also have fewer side effects when used appropriately.
Research supporting willow bark:
Studies show willow bark extract reduces lower back pain and osteoarthritis pain significantly compared to placebo. Effects are dose-dependent—higher doses work better.
A study using 240 mg salicin daily found significant pain reduction in people with osteoarthritis after two weeks of use.
Practical use:
Standardized willow bark extract providing 120-240 mg salicin daily, split into two or three doses. Take with food to reduce stomach upset.
Effects take several days to build—this isn’t immediate pain relief like pharmaceutical NSAIDs. Consistent use for at least one to two weeks before evaluating effectiveness.
Who benefits:
People seeking milder anti-inflammatory effects without pharmaceutical NSAID side effects. Those with chronic low-grade joint pain rather than severe inflammation.
Important cautions:
Don’t use willow bark if you’re allergic to aspirin or have bleeding disorders. The mechanisms are similar enough to create similar risks.
Don’t combine with blood thinners without medical supervision. Don’t use before surgeries—it affects clotting.
Stomach upset can occur, though less commonly than with aspirin. Taking with food helps.
Epsom salts (magnesium sulfate) in baths provide multiple potential benefits for joint pain, though mechanisms are debated.
Proposed benefits:
Magnesium absorption through skin may occur, though the extent is unclear. Magnesium has anti-inflammatory effects and many people are deficient.
Heat from the bath itself provides therapeutic effects—muscle relaxation, improved circulation, pain relief through thermal mechanisms.
Buoyancy in water reduces joint loading, allowing more comfortable movement and stretching.
The ritual and relaxation of bathing reduces stress, which independently affects pain perception.
Research status:
Evidence for transdermal magnesium absorption is mixed. Some small studies suggest it occurs; others are skeptical. The warm water effects are undisputed.
Many people report subjective benefit regardless of which mechanisms are responsible. Placebo effects plus thermal effects plus relaxation create real symptom relief.
Practical use:
Add 1-2 cups Epsom salts to warm bath. Soak for 15-20 minutes. Two to three times weekly for chronic pain management.
Water should be comfortably warm, not excessively hot. Very hot water can be inflammatory rather than therapeutic.
Use this as relaxation and self-care time. The psychological benefits complement any physiological effects.
Who benefits:
People with multiple painful joints who benefit from whole-body warmth. Those who find bathing relaxing and can incorporate it into routines.
Ginger contains gingerols and shogaols with genuine anti-inflammatory properties demonstrated in research.
How ginger works as a natural remedy for joint pain:
Ginger compounds inhibit inflammatory pathways, including COX and LOX enzymes. This reduces production of inflammatory prostaglandins and leukotrienes.
Antioxidant effects protect tissues from oxidative stress that contributes to inflammation and pain.
Some research suggests ginger affects pain perception through effects on serotonin and other neurotransmitters.
Research supporting ginger:
Multiple studies show ginger extract reduces osteoarthritis pain, particularly in knees. One trial found 500 mg twice daily as effective as ibuprofen for knee pain.
A systematic review concluded ginger has significant anti-inflammatory and analgesic effects, though optimal dosing needs more research.
Practical use:
Fresh ginger grated into tea, food, or smoothies. One to two inches of fresh root daily provides meaningful amounts of active compounds.
Ginger extract capsules standardized to gingerols: 250-500 mg twice daily. Effects build over days to weeks of consistent use.
Ginger powder in cooking works but fresh ginger or concentrated extracts provide more active compounds.
Who benefits:
People with osteoarthritis, particularly knees and hips. Those seeking natural anti-inflammatory support without pharmaceutical side effects.
Safety considerations:
Ginger is generally very safe. Some people get mild heartburn or digestive upset.
Ginger has mild blood-thinning properties. If you’re on anticoagulants, mention ginger use to your doctor, though normal culinary amounts are typically fine.
Tart cherry juice has anti-inflammatory and antioxidant properties that help some people with joint pain, particularly exercise-related inflammation.
Research on tart cherries:
Studies show tart cherry juice reduces muscle soreness and inflammation markers after intense exercise. Some research demonstrates benefits for osteoarthritis and gout.
The active compounds are anthocyanins and other polyphenols with anti-inflammatory and antioxidant effects.
Practical use:
Eight to twelve ounces of tart cherry juice daily. Use unsweetened versions—added sugar negates anti-inflammatory benefits.
Tart cherry extract capsules provide concentrated compounds without the liquid volume and calories.
Most effective when used consistently around times of increased activity or known inflammatory flares.
Who benefits:
Active people dealing with exercise-induced joint inflammation. Those with osteoarthritis seeking additional anti-inflammatory support.
People with gout may benefit from reduced uric acid levels with regular tart cherry consumption.
Considerations:
Tart cherry juice contains significant natural sugars and calories. Factor this into overall diet if weight management matters.
Effects are modest—helpful but not dramatic for most people. Works better as part of comprehensive approach.
Massage provides multiple mechanisms of relief beyond just feeling good.
How massage helps:
Increases blood flow to treated areas, supporting healing and reducing aching from poor circulation.
Reduces muscle tension around joints, which often contributes significantly to perceived joint pain.
Stimulates mechanoreceptors that can modulate pain signals through gate control mechanisms—touch sensations override pain sensations.
Releases endorphins and reduces stress hormones, affecting pain perception through central nervous system effects.
Research support:
Studies show massage reduces osteoarthritis pain, particularly in knees. Regular massage sessions produce cumulative benefits better than occasional treatments.
The type of massage matters less than consistency and pressure appropriate for your tolerance.
Practical application:
Professional massage: weekly or biweekly sessions focusing on affected joints and surrounding muscles. Swedish massage, deep tissue, or myofascial release all help.
Self-massage: daily brief sessions using hands, foam rollers, or massage tools on accessible joints. Five to ten minutes per area provides benefit.
Partner massage: have someone you trust work on hard-to-reach areas like upper back and hips.
Who benefits:
People with joint pain accompanied by significant muscle tension. Those who respond well to touch and find massage relaxing.
Important notes:
Avoid aggressive massage directly on inflamed joints—gentle work around the joint, not on it.
Some soreness after deep massage is normal. Sharp pain during massage means pressure is too intense.
Pain perception involves both physical and psychological components. Mind-body practices affect how your brain processes pain signals.
How meditation helps joint pain:
Reduces pain catastrophizing—the tendency to expect the worst and focus excessively on pain. This psychological pattern amplifies pain perception.
Activates descending pain modulation pathways—brain mechanisms that can dampen pain signals before they fully register as suffering.
Reduces stress and anxiety, which lower pain tolerance and worsen pain perception.
Improves sleep quality, which independently affects pain levels.
Research evidence:
Studies show mindfulness meditation reduces chronic pain intensity and improves function. Brain imaging reveals changes in pain processing regions.
A systematic review found meditation programs produce moderate improvements in pain and small improvements in function for people with chronic pain.
Practical implementation:
Start with guided meditation apps—Headspace, Calm, Insight Timer all have pain management programs.
Begin with 5-10 minutes daily. Consistency matters more than duration. Gradually increase as the practice becomes comfortable.
Body scan meditations specifically target awareness of physical sensations without judgment—particularly relevant for pain management.
Who benefits:
People whose pain worsens with stress or anxiety. Those open to psychological approaches alongside physical treatments.
Particularly helpful when pain is chronic and partially maintained by central nervous system sensitization.
Realistic expectations:
Meditation doesn’t eliminate pain but changes your relationship to it. Pain might remain but suffering decreases.
Benefits accumulate with consistent practice over weeks and months. Occasional meditation produces minimal lasting effect.
Acupuncture has genuine analgesic effects demonstrated in research, though mechanisms remain debated.
Proposed mechanisms:
Stimulates release of endorphins and other endogenous pain-relieving compounds. This is the most established mechanism.
May modulate inflammatory responses and affect nerve signaling in treated areas.
Produces measurable changes in brain regions involved in pain processing, visible on functional MRI.
Research support:
Multiple systematic reviews find acupuncture more effective than sham acupuncture for osteoarthritis pain, particularly knees.
Effects are modest but clinically meaningful for many people—roughly 20-30% pain reduction on average.
Real acupuncture appears more effective than “sham” acupuncture (needles in non-traditional points), suggesting specific point selection matters.
Practical considerations:
Seek licensed acupuncturists with specific training, not practitioners offering acupuncture as an add-on to other services.
Initial benefits often require 4-8 sessions. Single sessions rarely produce lasting effects.
Maintenance treatments every 2-4 weeks sustain benefits once initial improvement occurs.
Who benefits:
People with osteoarthritis, particularly knees. Those seeking non-pharmaceutical pain management options.
Some insurance covers acupuncture for certain conditions—check coverage before starting.
Important notes:
Acupuncture is generally safe when performed by qualified practitioners using sterile needles. Adverse effects are rare and usually minor.
Cost can be significant without insurance coverage. Weigh cost against likely benefit for your situation.

Yoga combines movement, stretching, strength building, and mind-body practices—multiple mechanisms in one intervention.
How yoga helps as a natural remedy for joint pain:
Improves flexibility and range of motion in joints that have become stiff from limited movement.
Builds strength in muscles supporting joints, reducing load on damaged joint structures.
Teaches body awareness and movement quality, often improving biomechanics that contribute to pain.
Includes breathing and meditation components that affect pain perception centrally.
Research evidence:
Studies show yoga reduces pain and improves function in people with osteoarthritis, particularly knees.
A systematic review found yoga comparable to physical therapy for knee osteoarthritis pain.
Practical implementation:
Gentle or restorative yoga styles work better than aggressive power yoga for joint pain. Yin yoga, gentle hatha, or chair yoga are good starting points.
Tell instructors about joint issues so they can offer modifications. Avoid poses that aggravate pain—honor your body’s signals.
Two to three sessions weekly provide benefit. Home practice using videos or apps works if studio classes aren’t accessible.
Who benefits:
People with mild to moderate joint problems who can safely perform modified yoga poses.
Those who enjoy movement practices and respond well to mind-body approaches.
Cautions:
Some yoga poses stress joints significantly if done incorrectly or before you’re ready. Get proper instruction.
Avoid hot yoga if you have inflammatory arthritis—excessive heat may worsen inflammation.
Sleep isn’t typically considered a remedy, but it profoundly affects joint pain through multiple mechanisms.
How sleep affects joint pain:
Growth hormone release during deep sleep supports tissue repair, including damaged cartilage and inflamed joint structures.
Sleep deprivation increases inflammatory markers throughout your body, worsening joint inflammation.
Poor sleep lowers pain tolerance—the same joint damage feels more painful when you’re sleep-deprived.
Sleep quality affects mood and stress levels, which independently influence pain perception.
Research evidence:
Studies consistently show poor sleep correlates with worse pain, higher inflammatory markers, and faster arthritis progression.
Improving sleep quality reduces pain intensity even when joint damage remains unchanged.
Practical implementation:
Prioritize 7-9 hours nightly. Not aspirational—actual sleep time. Track sleep to ensure you’re getting adequate amounts.
Sleep hygiene basics: dark room, cool temperature (65-68°F), consistent schedule, limited screens before bed, comfortable mattress and pillows.
Address sleep disorders if present. Sleep apnea, restless legs, insomnia all worsen pain and deserve treatment.
Pain-appropriate sleeping positions with proper pillow support reduce joint stress during sleep.
Who benefits:
Everyone with joint pain, but particularly those who notice pain worsens after poor sleep nights.
Addressing sleep is foundational—other remedies work better when sleep is adequate.

What you eat fundamentally affects inflammation levels throughout your body, including your joints.
How diet affects joint pain:
Certain foods consistently increase inflammatory markers—processed foods, excess sugar, omega-6 heavy vegetable oils.
Other foods reduce inflammation—omega-3 rich fish, colorful vegetables, olive oil, nuts, berries.
Shifting dietary patterns changes the inflammatory balance and measurably affects joint pain for many people.
Research support:
Mediterranean diet patterns reduce inflammatory markers and slow arthritis progression in multiple studies.
Specific foods like fatty fish demonstrate anti-inflammatory effects in controlled trials.
Practical implementation:
Focus on anti-inflammatory whole foods: fatty fish 2-3 times weekly, lots of vegetables, olive oil as primary fat, nuts, berries, whole grains.
Minimize processed foods, added sugars, and excessive omega-6 vegetable oils.
Don’t pursue elimination diets without cause. Balanced anti-inflammatory eating works better than restrictive approaches for most people.
Who benefits:
Everyone with joint pain, but particularly those with inflammatory arthritis or significant systemic inflammation.
Dietary changes work slowly—expect 4-8 weeks of consistent eating before noticing pain changes.
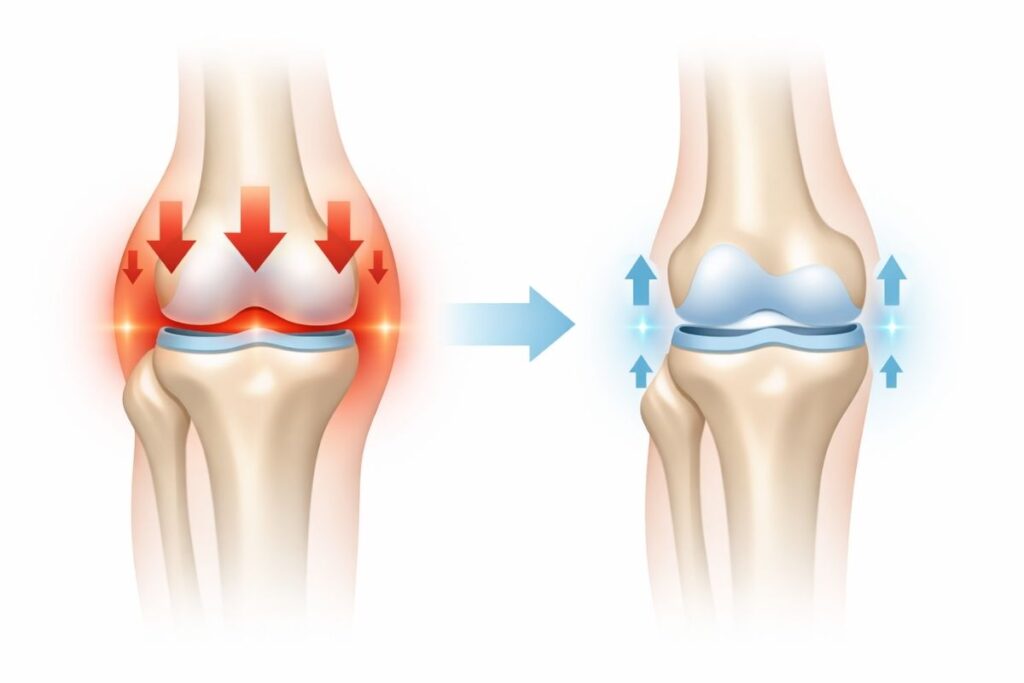
Weight management might seem obvious, but it’s one of the most powerful natural remedies for joint pain affecting weight-bearing joints.
How weight affects joint pain:
Every pound of body weight creates approximately four pounds of force on knees during walking. Losing ten pounds removes forty pounds of force—massive impact on joint stress.
Excess joint stress is especially damaging to the knees, which is why targeted strengthening and protective movement patterns are essential for long-term relief.
Fat tissue produces inflammatory compounds that circulate systemically, affecting all joints including hands and shoulders.
Excess weight worsens sleep apnea and reduces sleep quality, which independently worsens pain.
Research evidence:
Weight loss studies consistently show that even modest loss—10-15 pounds—significantly reduces knee and hip osteoarthritis pain.
Some research suggests weight loss slows cartilage loss and disease progression, not just symptom management.
Practical approach:
Even five to ten percent of body weight creates measurable benefits. A 200-pound person losing 10-20 pounds will likely notice significant improvement.
Gradual sustainable loss beats rapid aggressive loss. Focus on permanent habit change, not temporary restriction.
Combine dietary changes with appropriate exercise rather than relying solely on calorie restriction.
Who benefits:
Anyone carrying excess weight with knee or hip pain. Benefits are dramatic and often exceed pharmaceutical interventions.
These fifteen natural remedies work best in strategic combinations, not isolation.
Daily foundation:
Symptomatic relief tools:
Supplementary practices:
Targeted additions:
The most effective approach uses multiple complementary remedies addressing different aspects of joint pain rather than searching for single magic solutions.
Natural remedies for joint pain work within limitations. They help manage symptoms, support healing, and reduce reliance on pharmaceuticals. They rarely “cure” significant joint damage. Realistic expectations paired with consistent application creates the best outcomes.
Note: This is educational information about natural remedies for joint pain, not medical advice. Natural doesn’t mean risk-free—consult healthcare providers before starting new treatments, especially if you have medical conditions or take medications.